If you haven’t heard of an APCD, it’s one of those acronyms you need to know. All-Payer Claims Databases are simply databases that consist of claims data from all health care payers in a given state. This includes private payers such as Blue Cross Blue Shield, and public payers such as Medicaid or Medicare. As you can imagine, it’s a lot of data, and it certainly fits the mold of “big data.” Moreover, APCDs are setting the stage for data-driven healthcare and big analytics.
Colorado’s APCD website recently went live and I spent some time playing around with the maps and report generation tools. It’s great to see population health and health metrics visually, and Colorado is to be commended for its APCD’s public interface. Giving the public access to this information will empower Colorado’s citizens to make better decisions about their health care.
All that’s been done with APCDs to-date is great, but on my team of analytics-obsessives, we like to continuously ask the question “so what?” What does that mean to the policy maker, the end user, and ultimately to the recipient of services? Now that we have all of this information in one place, how are we maximizing its use to essentially transform a system? With the data in the APCD there are certainly a lot of decisions on the payer, provider, and patient level that can be made. For instance, payers can identify what they’re spending the most on, providers can modify their treatments to be more effective, and patients can be empowered to make better choices. But, what does this mean to really enhancing quality and reaching our ultimate goal of improving health? This where the opportunity to leverage analytics comes into play. Not just any analytics, but advanced analytics. Predictive analytics.
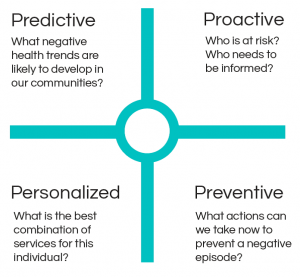
APCDs offer us the ability to be predictive, proactive, preventive and personalized, or what I like to call the 4 P’s of quality care. The first ‘P’ is critical because when we can use the data in our APCDs to predict, we can increase their value tenfold and it becomes a tool in transforming care. While states have a road ahead of them to reach this point, and the dissemination of this data will require more engagement from providers, payers, and patients, big analytics is the direction APCDs are headed. And states can start now by using predictive analysis alongside their current reporting methods.
For example, we can utilize the data to forecast developing health trends and project their costs to the system one, three or five years down the road. Or, we can predict which groups of patients are at-risk for a chronic illness, like high blood pressure or arthritis. As APCDs are expanded to integrate clinical and financial data through linkages with health information exchanges (HIE) and health insurance exchanges (HIX), they will facilitate big analytics to support personalized care, improve health outcomes and reduce costs to our system.

3 Comments
Thank you very much Krisa! I can say first hand from my experience in the Northeast States that APCD's are quickly gaining traction. In my region alone, every state in New England as well as New York have APCD's which are either in development or seeking RFI/RFP responses to ready themselves. In addition, having spent much time with the National Association of Health Data Organizations and the APCD council I can safely say that APCD's are a nation wide priority in the public govenment space. In my experience, thus far, I have seen a great amount of emphasis on Information management, Reactive Analytics, and Business Intelligence. There is no question that these areas are profoundly important as it relates to APCD's. However, I believe a vital ingredient is missing in this recipe, that of Preditive Analytics. I thank you very much Krisa for helping to illustrate this point above and driving home the importance and value of predictive analytics in APCD's. I know Krisa and I have spent a good deal of time and effort on APCD research/responses and we hope to see a great amount of SAS involvement/growth in the APCD movement.
The best of predictions don't always pan out. So don't we need a step in the loop for failure? The risk our prediction's false?
Yes, it's imperative to utilize data quality tools to ensure the integrity of APCD reporting and predictive analysis. Good data is the key to any effective analysis. Moreover, as predictive models are built, they ‘learn’ from each other to become ‘smarter,’ and as more data is added, the accuracy is also enhanced. I think APCDs are ideal for making larger-scale predictions on population health and segments of the population. Linkages with clinical datasets (i.e. HIE) will facilitate better analysis and predictions at the individual level.