 The expletive leapt from the lips of the orthopedic surgeon as he entered my hospital room. He was swathed in a green gown, purple gloves, and a white surgical mask – for his protection, not mine. He was clearly upset.
The expletive leapt from the lips of the orthopedic surgeon as he entered my hospital room. He was swathed in a green gown, purple gloves, and a white surgical mask – for his protection, not mine. He was clearly upset.
“What, exactly, does $#@! mean?” I asked.
“It means you’re having surgery tomorrow.” he replied.
“Oh, this isn’t really a good time for me,” I answered. “I just started a new job, my husband has to go out of town this weekend, we just moved to a new house….”
“Perhaps I didn’t make myself clear,” he interrupted. “Either you’re having surgery tomorrow, or you’re going to die.”
Well, when he put it THAT way…
The last resort
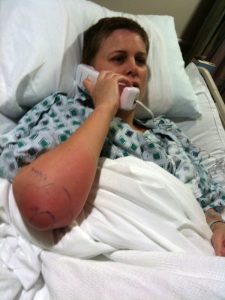
It was my third day in the hospital, confined in isolation. I had arrived by ambulance over the weekend with tendrils of inflammation extending from my elbow to my shoulder. The angry red lines represented a very serious infection, septic arthritis with systemic symptoms of sepsis, that caused my blood pressure to nosedive and my body to mount an all-out war to save itself. My elbow had swelled to double its normal size, as the ferocious bacteria waged war inside it against the combined defenses of my immune system and the strongest last-resort antibiotics available. The surgeon explained what I had intuitively known from the moment I had first noticed the crawling redness: If the infection spread past my shoulder, they would be out of medical options to help me fight it. And it seemed that in spite of the powerful antibiotics being used in combination, nothing was stopping this infection from creeping up my arm in its bid to take over my whole body. My life was in danger, and the surgeon explained that amputation - removing the arm entirely - might end up as the last option left to save me. As terrifying as that was, it seemed the better of two options – exchanging my arm for the chance to keep my life.
His bedside manner – the cursing, the bluntness – actually amused me. I preferred those straightforward answers to the worried glances and soft murmurings behind closed doors that the nurses and other staff seemed to favor. I thought of the many experiences I had had with doctors of varying skills over the years. My husband is a professor at a medical school, and thus I had often encountered newbie interns, residents just getting comfortable in their profession, and the attending physicians who were mentoring them all.
Sure enough, a first-year resident was assigned to the team managing my situation. He was determined to throw every technology in the book at the problem: Run this lab test! Get this scan! Have an MRI! The resident was confident that the answers would lie in those sensor readings, confident that the tests would tell him precisely what was wrong, confident that the data alone would tell him what to do next. I overheard him mumbling with another specialist in the hall, completely lost: “I have no idea what to do. The drugs just aren’t working.”
As it turned out, I was spared the surgery. That night, the front line of the infection stopped advancing and the surgeon called off the procedure, clearly relieved. And in the next few days, the infected area slowly shrank in size as the bacteria pulled back from their offensive. The doctors drew smaller concentric circles on my arm each day, tracking the steady retreat of the invaders like generals with battlefield maps.
However, I now encountered a new health challenge: An overwhelming allergic reaction to the powerful intravenous antibiotics. I developed a high fever, and an ugly red rash bloomed all over my body from the tops of my ears to the tips of my toes. The resident, the hospitalist, the surgeon, and the infectious disease specialist were all at a loss. Their tests and their tools were useless in the face of variables they had not yet encountered. They could see what was happening, but they couldn’t understand it – it was all happening too fast, and there were too many things to think about. Each of them had a narrow perspective, blinded by the boundaries of their specialties. They had no context with which to understand my dilemma.
Saved by experience and context, not more data
So they called in the expert, a very senior internal medicine specialist who had moved to the US decades ago after years of healing difficult cases with the Russian military. Calm, wise, and unflappable, he canceled a full morning schedule to see me on an emergency basis. He did not order any new lab work. He asked for no additional scans.
Instead, he listened. He listened and he analyzed for a full hour, asking questions, making notes, investigating variables from my diet to my family history to my travel patterns. He slowed things down, meeting each moment as it came, carefully observing me, and my swollen arm, and the information in my medical record, in context. He analyzed what he heard through the lens of his experience, requesting new information as needed, disregarding elements that he found to be irrelevant – including some of the lab work ordered by the resident over the course of the week. And at the end of that magical hour, he steepled his fingers together, smiled a slight smile, and said, “I have seen this before. I know what is wrong with you. I know what we can do here.”
And so he did. He got the answers he needed to return me to health not from a sensor reading, not from a scan, not from the latest device, but from decades of experience seeing cases like mine – perhaps not precisely the same presentation, but sufficiently similar that he was able to filter the signal from the noise. It turned out that I had a rare condition that none of the countless hospital tests could possibly identify, but which an expert with the pattern of data and the motivation and insight to ask the right questions of the data could discern. Certainly he needed the raw data from the existing tests, needed to know what they had ruled out, to help focus his decisions and planning. But the life-saving magic came through his analysis – from comparing my case to those he had seen before, and predicting which intervention would give us the result we all wanted – my return to a normal life.
Within weeks, I had returned to work. A few months later, I was able to use my arm normally again. I am well aware of how fortunate I am. Sepsis kills 590 people each day in the United States alone.
The Internet of Things
I don’t dwell on what happened, but it did come to mind recently as I was trying to explain to a colleague outside of my field how SAS software is unique in the world of the Internet of Things, or IoT as it is called. IoT is a relatively recent phenomenon in the worlds of manufacturing, energy, smart cities, healthcare, and retail. Essentially IoT refers to the concept of everyday objects – from industrial machines to wearable devices – using built-in sensors to gather data and take action on that data across a network. Elements of it, including many of the sensors and some rudimentary processing, have been around for many years. What has changed is the volume, variety, and velocity of that data. Cisco has projected that there will be 50 billion connected devices by 2050, sending and receiving data in a variety of formats.
Another thing that has changed is that organizations are realizing that the effective use of that data is essential to their very survival – and many are at a loss as to what to do.
Less experienced organizations – the first-year residents of the business world – are throwing technology at the problem. They fervently hope that the answer lies in more tests, more sensors, more gadgets, more data! In many cases they may already have all the data they need, but without the ability to filter it and put it in meaningful big-picture context, and doing this fast, they cannot diagnose or address what is draining their energy and profit potential.
When it matters - have an expert on call
How valuable it is, then, to have an expert on call – an expert with decades of wisdom, who has seen this all before, who is not overwhelmed or distracted by the torrents of data. If the survival of my organization depended on uncovering patterns in my IoT data, I can think of no one more suited to the challenge than the experts at SAS. For forty years, they have been uncovering hidden patterns in data, using the insights to improve lives in areas as broad as saving lives after earthquakes, fighting fraud, developing new health solutions, protecting wildlife, improving sports experience, manufacturing quality products, and keeping energy flowing. These decades of experience, with different types of data from different contexts, enable them to bring a certain art to the science of analytics – a creative approach grounded in a deep foundation of problem solving.
And I am alive to help make this happen. I was fascinated to learn that SAS software has been used to investigate effective treatments for the very infection – methicillin-resistant staphylococcus aureus (MRSA) – that almost took my life. I am grateful to work for an employer that does so much to improve lives, and whose work may have contributed to saving mine.
I was inspired to write this blog post when I learned of the upcoming Step on Sepsis walk taking place on May 7 in Cary, North Carolina, very close to my office. It is an issue that touches more lives than you might think.
“It is more common than heart attack, and claims more lives than any cancer, yet even in the most developed countries fewer than half of the adult population have heard of it” (World Sepsis Day FAQ Sheet).
Early action is critical
Familiarize yourself with the signs and symptoms of sepsis, either through educational materials like those from the CDC or through unique (and amusing) YouTube videos. Early action is critical. Learning to filter the signals of sepsis from the background noise of common symptoms can make a life-saving difference for you or someone you love.

7 Comments
Well written, Marcia.
Oh my goodness! Thanks for sharing your experience and highlighting the valuable role data aand analytics has in our lives.
I was on the edge of my seat reading this, even though I know you're now okay. Thank you for sharing your story.
Marcia, thank you for sharing your story! MRSA is so scary and it's awesome that you had the help you did. We're glad you're here with us at SAS to tell your tale and provide the real-life example of analytics makes a difference!
Any one can add hay to the hay stack. Only experts can find the needle in the hay stack. Thank you for making big data analytics so interesting to read.
Your story hit home for me, Marcia. Twelve years ago I had a son who was born with a very rare skin disorder. The staff at the hospital had no idea what it was or how to treat it. He was given pain medication and my husband and I were told he would likely die within the week. Two very difficult days later he was seen by a specialist who took one look at him and gave us that moment of peace we greatly needed. "I know exactly what this is, (and as long as we can avoid infection in these early weeks) he will survive and live a very full life." I am forever grateful for the experience of that doctor, and am excited to work for a company that can help our health care professionals gather and share that data, so the next neonatologist to encounter this disease can effectively treat the child right from the start, and give the anxious new parents accurate information and hope for their baby's future. Even if they haven't actually encountered the disease in practice before.
Amazing! Thank you for sharing your story.