Healthcare fraud is alive and well. Honesty is dead and gone. There, I’ve said it. What else are we to take from surveys that find that 27% of people would sell their work passwords...44% of them for less than $1,000?* What does it mean that 37% of survey respondents think lying on a resume is fine, and 24% of men support cheating on your taxes?**
We're in the midst of International Fraud Awareness Week, which is about finding solutions to fraud. So we don’t have time for honesty's eulogy now, but acknowledging our loss is the first step to moving on. It’s time to do something about it.
Experts look to others in their field to learn, test ideas and share methods. That approach is a best practice, and one I strongly support. But, in a post-honesty world, threats are everywhere. Learning from other industries and adapting their methods to healthcare fraud risks is past due.
Government has seen attacks increase dramatically with the rise of identity theft. Government tax and benefits programs are now the second highest use of stolen identities behind banks.
Insurance companies have learned to partner with their competitors when fighting fraud, forming consortia to share data on high risk claims and claimants.
Show me the money
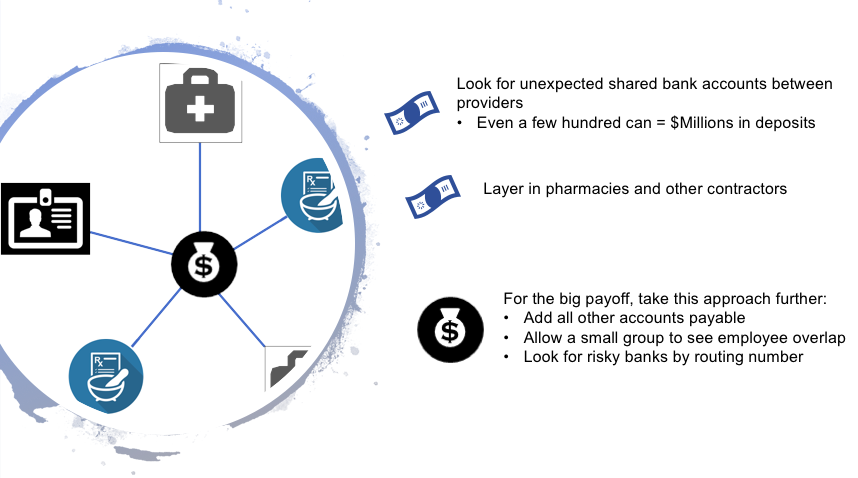
Taking a page from banking, look at anti-money laundering (AML) efforts. At a basic level, it's about ownership of accounts, connections between ownership, and money flows.
In healthcare, experts regularly look at connections between patients and providers, referring providers and pharmacies. But, we typically ignore where the money is deposited. Diving into details on money flows can easily make previously unknown connections.
Ghost in the machine
Government tax agencies have learned from fighting identity theft that machine generated data is vital to analysis. Machine generated data ranges from the IP address of tax returns filed online, to the exact time stamp that return was received.

Healthcare organizations tend to ignore this data, or don't have access to it for fighting fraud. Analysis of this data can make a leap forward in the post-honesty world:
These ideas are just the beginning. Look beyond your own walls. Think about how Visa, or Geico, or Amazon, are fighting fraud today. Those ideas can be turned back towards healthcare. They are the core of using analytics and machine learning to stem the tide in the post-honesty world.