 Let’s face it. Data sharing between platforms in health care just isn’t easy. Patient data privacy concerns, incompatible file formats, asynchronous identifiers … I’ve heard it all. From the electronic health record (EHR), picture archiving and communication systems (PACS) to discrete processes like pharmacy or departmental information systems, achieving some level of integration seems like a pipe dream. So where does this leave the analyst who wants to solve complex issues related to improving health outcomes?
Let’s face it. Data sharing between platforms in health care just isn’t easy. Patient data privacy concerns, incompatible file formats, asynchronous identifiers … I’ve heard it all. From the electronic health record (EHR), picture archiving and communication systems (PACS) to discrete processes like pharmacy or departmental information systems, achieving some level of integration seems like a pipe dream. So where does this leave the analyst who wants to solve complex issues related to improving health outcomes?
Achieving analytic interoperability
Having a view of all our health care interactions in one place was the goal of the electronic health record. The dream was that a patient would not have to answer the same questions for each new doctor or clinic because there would be complete access to all our medical history. This has yet to materialize, even in the most connected and simplified health care settings.
To further complicate matters, much of the data that would be useful to medical providers isn’t specific to patient health. Social determinants, including education and environmental exposure, along with fitness tracking and other new data are not yet regularly used to drive better health outcomes.
In reality, most of today's analytic projects could be described by the graphic below. In this scenario, the EMR is a primary source of patient data, but it's combined with other third party and proprietary data sets to arrive at an analytic data set that supports predictive modeling and AI.
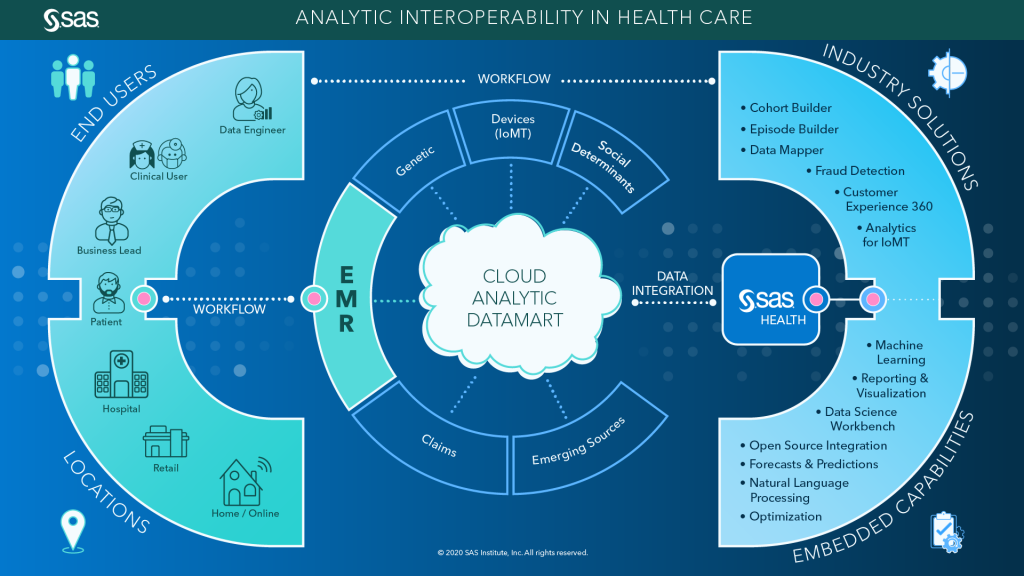
Analytic interoperability occurs when relevant patient data is brought together and delivered through one access point with one goal in mind: better outcomes. It allows the caregiver to better understand the patient; operations and financial leadership is better able to plan; and it aligns the network of providers, both new and old, to the needs of the population they serve and the channels they operate.
Analytic interoperability is driven using standards, including FHIR, DICOM, HL7 and other proprietary coding sets utilized within the health care world. However, standards do not enforce data quality. The lack of trustworthy and timely data is still a barrier to many analytic projects.
Benefits of analytic interoperability
As with other industries, there's an increasing interest in data driven decisions throughout the health care system. As we see a growing need to collaborate among care providers, operational staff, executive leadership and the new players in health care, there's a corresponding need for data consistency and access. Convergence between health and the pharmaceutical industry, as well as an increase in retail-driven health care, creates the need to share data.
One simple benefit of this approach is in medication. Interoperable health care provides a clinician with an accurate and timely medication list without relying on patient recall. This information helps prevent the prescription of contraindicated medications, allows tracking through the pharmacy and helps avoids potential high-cost emergency care.
Another example is bringing data from home devices into the hospital to manage chronic conditions remotely, such as diabetes. Predicting the next patient intervention and applying preventative measures to help keep them at home and well is a direct result of analytic interoperability.
How does SAS enable analytic interoperability?
SAS can assist throughout the journey to analytic interoperability. Whether it's wrangling the data, providing the industry solutions or creating the platform for advanced analytics, SAS can help create better insights for patients and health care staff, whether clinical, operational or technical.
Because the cloud is now more accessible to the health care industry, there has never been a better time for interoperability in all aspects of care. Linking data together to create the 360-degree view of the patient and their health ecosystem will contain costs, improve quality and increase access to health care.
Learn more at sas.com/healthcare.

1 Comment
Thanks for sharing the informational healthcare blogs.